Your Journey to Allergy & Asthma Freedom
Schedule an
Appointment
Allergy relief is just a click away. Our board-certified allergists and advanced practice providers are ready to listen to you and help you feel better.
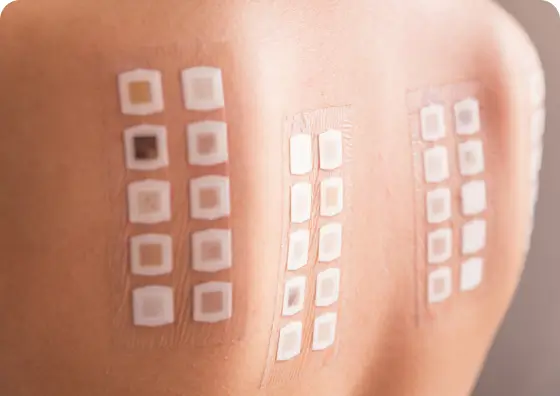
Understand Your
Symptoms
We offer a variety of diagnostic tests to find out what causes your symptoms so that we can treat the real problem and fully understand your condition.
Get Personalized
Treatment and Relief
Personalized treatment plans help 90% of patients with seasonal allergies and 70–80% of patients with perennial allergies get better.
ABOUT PREMIER ALLERGIST

ABOUT PREMIER ALLERGIST
For nearly 30 years, Premier Allergist, now part of the AllerVie Health network, has been providing exceptional allergy, asthma, and immunology care to patients in Maryland, Pennsylvania, Virginia, and Washington DC. Serving over 30 locations in the northeast region, we prioritize patient-centered care, ensuring we are accessible and available whenever you need us.
Patient Resources
We want to make your experience with Premier Allergist as seamless as possible, so we've put together various resources to help make your journey smoother.
patient forms
Looking for something specific about your local clinic?
Please see the nearest location to find details about the clinic in your area.
Conditions We Treat
Learn more about the allergy, asthma, and immunological disorders that we treat. We believe that a clear understanding of your health condition and the terminology used by our allergists and advanced practice providers is key to finding the relief you need and freedom you deserve!
Ready to make an appointment?
Premier Allergist providers are ready to help you reclaim your life and start feeling better. Make an appointment today to start your journey to allergy and asthma relief.
locations near you

Looking For A Rewarding Career?
Change Your Life, and the Lives of Others
Join us and be part of a team that’s all about achieving personal success and changing lives! We’re a group of innovative physicians, experienced clinical staff, and administrative support teams who wake up excited every day to tackle new challenges. Our mission is to improve patients’ health and quality of life, and we can’t wait to have you on board!